Following is the full transcript of MIT professor Hugh Herr’s TED Talk titled: “How We’ll Become Cyborgs & Extend Human Potential.”
You can also listen to the MP3 audio: How we’ll become cyborgs and extend human potential – Hugh Herr at TED Talks
TRANSCRIPT:
I’m an MIT professor, but I do not design buildings or computer systems. Rather, I build body parts, bionic legs that augment human walking and running.
In 1982, I was in a mountain-climbing accident, and both of my legs had to be amputated due to tissue damage from frostbite. Here, you can see my legs: 24 sensors, six microprocessors and muscle-tendon-like actuators. I’m basically a bunch of nuts and bolts from the knee down.
But with this advanced bionic technology, I can skip, dance and run. Thank you.
I’m a bionic man, but I’m not yet a cyborg. When I think about moving my legs, neural signals from my central nervous system pass through my nerves and activate muscles within my residual limbs. Artificial electrodes sense these signals, and small computers in the bionic limb decode my nerve pulses into my intended movement patterns.
Stated simply, when I think about moving, that command is communicated to the synthetic part of my body. However, those computers can’t input information into my nervous system.
When I touch and move my synthetic limbs, I do not experience normal touch and movement sensations. If I were a cyborg and could feel my legs via small computers inputting information into my nervous system, it would fundamentally change, I believe, my relationship to my synthetic body.
Today, I can’t feel my legs, and because of that, my legs are separate tools from my mind and my body. They’re not part of me. I believe that if I were a cyborg and could feel my legs, they would become part of me, part of self.
NeuroEmbodied Design
At MIT, we’re thinking about NeuroEmbodied Design. In this design process, the designer designs human flesh and bone, the biological body itself, along with synthetics to enhance the bidirectional communication between the nervous system and the build world.
NeuroEmbodied Design is a methodology to create cyborg function. In this design process, designers contemplate a future in which technology no longer compromises separate, lifeless tools from our minds and our bodies, a future in which technology has been carefully integrated within our nature, a world in which what is biological and what is not, what is human and what is not, what is nature and what is not will be forever blurred. That future will provide humanity new bodies.
NeuroEmbodied Design will extend our nervous systems into the synthetic world, and the synthetic world into us, fundamentally changing who we are. By designing the biological body to better communicate with the built design world, humanity will end disability in this 21st century and establish the scientific and technological basis for human augmentation, extending human capability beyond innate, physiological levels, cognitively, emotionally and physically.
There are many ways in which to build new bodies across scale, from the biomolecular to the scale of tissues and organs. Today, I want to talk about one area of NeuroEmbodied Design, in which the body’s tissues are manipulated and sculpted using surgical and regenerative processes. The current amputation paradigm hasn’t changed fundamentally since the US Civil War and has grown obsolete in light of dramatic advancements in actuators, control systems and neural interfacing technologies.
Proprioception
A major deficiency is the lack of dynamic muscle interactions for control and proprioception. What is proprioception? When you flex your ankle, muscles in the front of your leg contract, simultaneously stretching muscles in the back of your leg.
The opposite happens when you extend your ankle. Here, muscles in the back of your leg contract, stretching muscles in the front. When these muscles flex and extend, biological sensors within the muscle tendons send information through nerves to the brain. This is how we’re able to feel where our feet are without seeing them with our eyes.
The current amputation paradigm breaks these dynamic muscle relationships, and in so doing eliminates normal proprioceptive sensations. Consequently, a standard artificial limb cannot feed back information into the nervous system about where the prosthesis is in space. The patient therefore cannot sense and feel the positions and movements of the prosthetic joint without seeing it with their eyes. My legs were amputated using this Civil War-era methodology.
I can feel my feet, I can feel them right now as a phantom awareness. But when I try to move them, I cannot. It feels like they’re stuck inside rigid ski boots.
Agonist-Antagonist Myoneural Interface (AMI)
To solve these problems, at MIT, we invented the agonist-antagonist myoneural interface, or AMI, for short. The AMI is a method to connect nerves within the residuum to an external, bionic prosthesis.
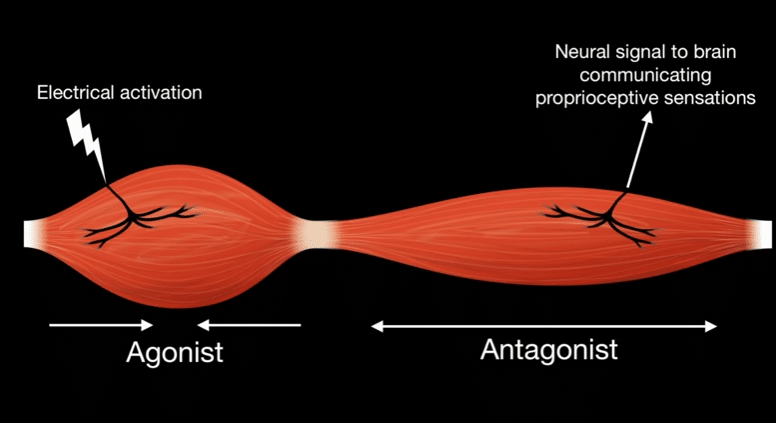
How is the AMI designed, and how does it work?
The AMI comprises two muscles that are surgically connected, an agonist linked to an antagonist. When the agonist contracts upon electrical activation, it stretches the antagonist. This muscle dynamic interaction causes biological sensors within the muscle tendon to send information through the nerve to the central nervous system, relating information on the muscle tendon’s length, speed and force.
This is how muscle tendon proprioception works, and it’s the primary way we, as humans, can feel and sense the positions, movements and forces on our limbs. When a limb is amputated, the surgeon connects these opposing muscles within the residuum to create an AMI.
Now, multiple AMI constructs can be created for the control and sensation of multiple prosthetic joints. Artificial electrodes are then placed on each AMI muscle, and small computers within the bionic limb decode those signals to control powerful motors on the bionic limb.
When the bionic limb moves, the AMI muscles move back and forth, sending signals through the nerve to the brain, enabling a person wearing the prosthesis to experience natural sensations of positions and movements of the prosthesis.
Can these tissue-design principles be used in an actual human being?
A few years ago, my good friend Jim Ewing — of 34 years — reached out to me for help.


